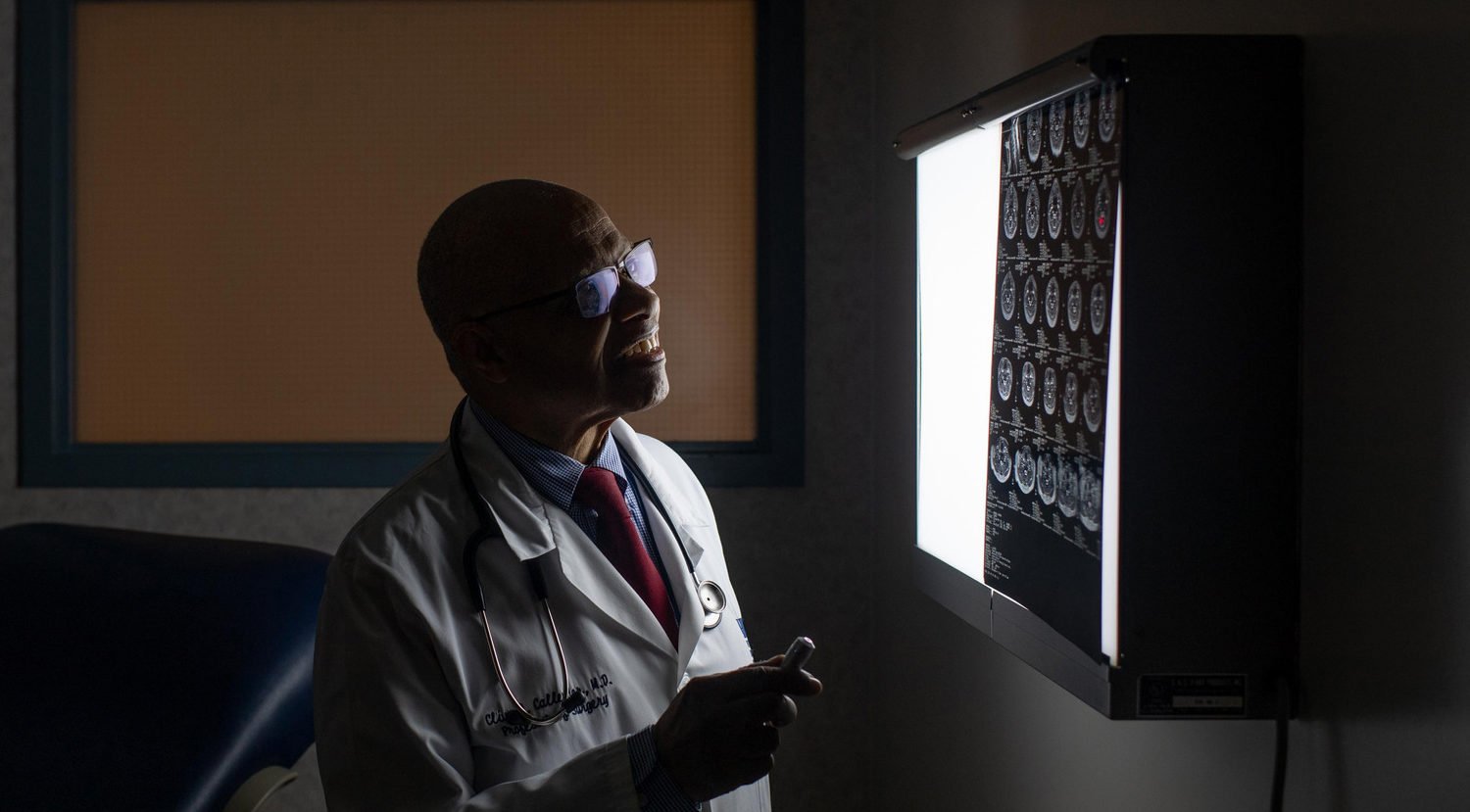
Unfortunately, it happens. That scrumptious dinner of chicken and chili peppers in Brazil could leave you in the fetal position on your hotel bathroom floor. Or, after days exploring Hong Kong in sandals, you may find that one toe has swollen up like a strawberry, making it painful to walk. Perhaps you’ll get feverish and chilled after mosquitoes lunch on you in Serengeti National Park.
To help prevent illness—and to know what to do when it strikes—doctors urge people who are bound for more exotic foreign realms to consult travel-medicine specialists beforehand. Such specialists—often nurses or physicians—pro-vide vaccines and other medicines to ward off disease, make risk assessments specific to your destination, and offer recommendations for avoiding and managing travel-related health issues. While a family physician can administer the same preventive shots, a travel-medicine specialist is more likely to have the vaccines on hand and to be up to date on requirements and diseases in specific countries.
People who travel internationally—for pleasure or for work—risk a host of illnesses. For every 100,000 business travelers who visit a developing country for one month, half will experience a health problem while there, with 8,000 needing a physician, according to the CDC Foundation, a nonprofit organization that partners with the federal Centers for Disease Control and Prevention. Yet just 10 percent of international business travelers seek preventive care before setting foot on a plane.
Travel medical care reaches beyond dispensing Cipro. The International Society of Travel Medicine includes more than 3,500 members in 100 countries, such as scientists who study the Zika virus, pharmacists offering vaccines, wilderness doctors who manage people with altitude sickness, and physicians specializing in tropical medicine who care for returning travelers stricken with illnesses such as dengue fever.
Why see someone who specializes in the field? Because disease spreads faster than ever, says Phyllis Kozarsky, professor of medicine and infectious disease at Emory University, who helped found the society in 1991. Thanks to air travel, someone can contract Ebola in Sierra Leone and potentially spread it to many others in a day—putting you at risk if you’re on that plane, not to mention your loved ones once you get home.
That’s where travel-medicine specialists come in. The Centers for Disease Control and Prevention (CDC) recommends that four to six weeks before embarking, patients visit such a specialist or a doctor familiar with travel medicine to get recommendations on vaccines, prophylactic medicines, and potential illnesses in the countries to be visited. Some local and county health departments provide pre-travel care—you can search for clinics through the CDC’s website—and some insurance policies cover pre-travel medical care.
Doctors and nurses who are trained in the specialty follow the latest information about vaccines required by particular countries. They can advise about medicines such as those that prevent malaria and gauge how they might interact with your current medicines. Sometimes proof of vaccines must be shown upon landing, and the requirements can change quickly depending on local health issues. Standard requirements of many countries include vaccines to prevent polio; hepatitis A and B; and measles, mumps, and rubella. Travel-medicine specialists such as those at Passport Health—which has multiple area locations—provide an International Certificate of Vaccination or Prophylaxis, commonly called a yellow card, listing the vaccines a patient has received and when.
In addition, the doctor or nurse will review a traveler’s risk for malaria, tuberculosis, and other diseases. The specialist can offer advice on taking precautions with food and beverages to avoid intestinal bugs, how to ward off mosquito bites that can cause dengue fever or malaria, and preventing and planning against safety risks, such as when you’re making high-altitude treks.
At Passport Health, clients discuss a trip with a registered nurse travel specialist, who comes up with a plan—including specific advice for those who have preexisting conditions.
“Preparation is the key,” says Lisa Maragakis, an epidemiologist and associate professor of medicine at the Johns Hopkins Health System. “If you’re going to be in an area without adequate health care, figure out what resources you’ll need. Have a plan.”
Suzanne Sataline (@ssataline on Twitter) writes from New York and has been sick in many countries.
This article appears in the May 2016 issue of Washingtonian.