About Coronavirus 2020
Washingtonian is keeping you up to date on the coronavirus around DC.
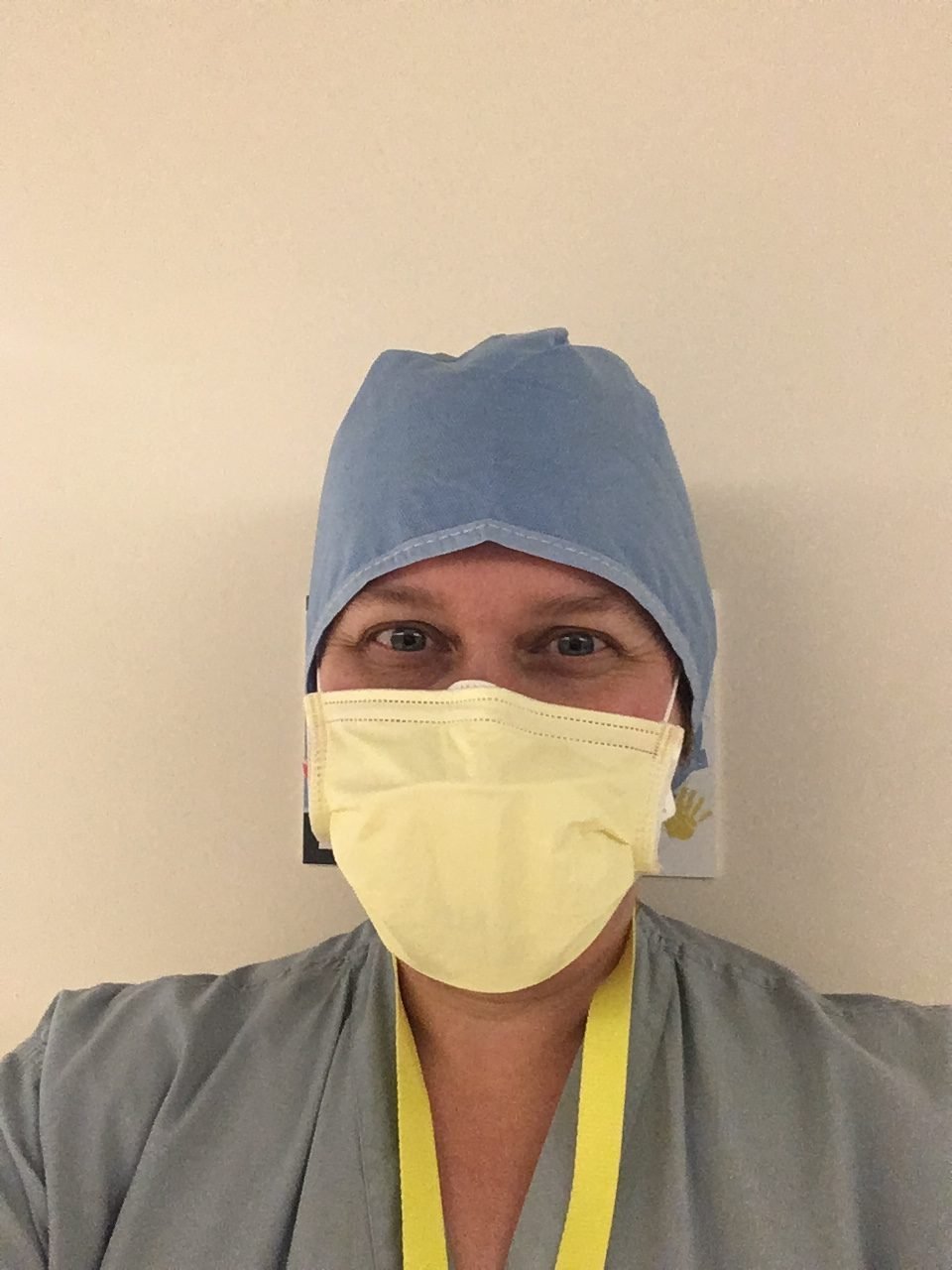
Elizabeth Montgomery, 44, of Centreville, is a nurse in the medical/surgical ICU at Inova Fairfax Hospital. We spoke to her on Friday, March 27.
“We have seen our patient population dramatically increase. We have 18 beds. I think all but three are now Covid-positive or rule-out patients. ‘Rule-out’ meaning we’re waiting for tests to be back. We’re seeing an increase, at least in our unit of patients, who need advanced respiratory care for presumed Covid or confirmed. Our bread and butter is respiratory, which is why we were deemed the designated unit for Covid patients.
“Everybody keeps saying this is like the flu, this is like the flu. It is not the flu. I want to be very clear on that. We’re very comfortable taking care of flu patients. These patients behave completely differently. And we are using more advanced treatments earlier. We have used early ventilator use, we have done ECMO—extracorporeal membrane oxygenation—which is basically a lung bypass, an artificial lung. We had never done that in this unit before. We also sometimes have to flip patients over onto their stomachs to improve oxygenation. In the bad flu seasons, we might do that once a week at the most. We’ve had three or four patients that have needed that this week. So these patients are requiring the highest level of respiratory care that we can provide.
“We are rationing supplies. We are trying to use one of the N95 masks per shift, per nurse. We had been using them one time per entry into a room. Basically, they were disposable. But that is no longer the case. The hospital is providing us with scrubs to wear while we’re here. So we change into the hospital scrubs at the beginning of our shift and then we can wear them here, take them off here, they’re laundered here. Personally, I’m just going straight home, trying not to touch anything, going directly into the shower, washing my hair every night, which I don’t normally do, and wiping everything down that I bring home with me. My phone, my shoes, anything.
“We are feeling the support from the community, and that is helping. Families are providing us with meals. Girl Scouts delivered cookies yesterday. It is stressful fielding a lot of family phone calls. We thought it might be a little better not having families actually on site, [but now] we’re dealing with multiple phone calls a day from families, which is appropriate. They’re scared, too.
“I’m not nervous so much about my health as I am my mental health. There’s a lot of unknowns with this disease. Every day we’re dealing with something different. ICU nurses are rarely afraid of what we encounter in a day. I think we are afraid of what might be coming. We do have nurses who are concerned about taking it home to their families, who have grandparents or parents living with them, who have young children who don’t understand that Mommy needs some distance right now. It’s the fear of what happens when we look like New York? What happens when we look like Italy? We’ll be fine as long as we can keep our protective gear supply where we need it to be. If we don’t have enough gear, that will take a huge toll on mental health.”
Interview has been lightly edited and condensed for clarity.