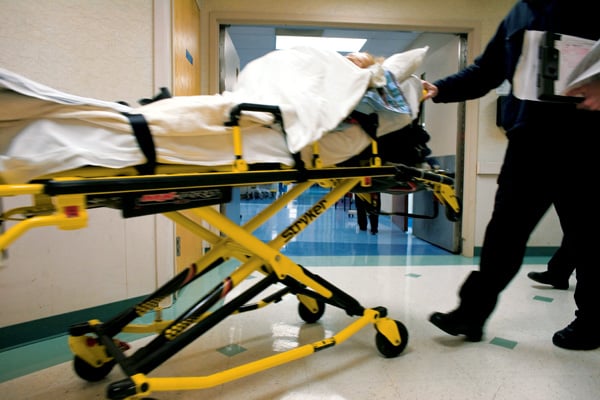
Here’s how to endanger and frustrate people going to a hospital emergency room for care. First, increase the number of ER patients and decrease the number of hospital emergency departments. Then cut the number of hospital inpatient beds—this will delay moving ER patients who need to be hospitalized into inpatient beds, which will create more ER crowding. To make things more chaotic, decrease the number of nurses and on-call specialists. Do all this, and you’ll have accomplished what our healthcare system has done—created uncertain, sometimes dangerous conditions in the ERs of even our best hospitals.
Just ask 36-year-old Marnie Abramson. For her, it began with an upset stomach around 8 on a Saturday night. She tried to sleep but awoke at midnight feeling very sick. She called her doctor, who told her to go to a hospital emergency room if she didn’t feel better in an hour. When she didn’t, she went to George Washington University Medical Center.
“When I got to GW at around 2 am, the ER waiting area was packed with 40 or more people,” she says. “There wasn’t a seat to be had. There was a young guy bleeding with a broken nose and a woman who said she thought she was having a heart attack who was filling out a form. I waited an hour and still hadn’t been seen by anyone. I felt a little better, so I thought, ‘This is ridiculous,’ and decided to go back home. Just as I was getting into my car, the pain and nausea hit me again and I started throwing up.”
Abramson, director of marketing for the Tower Companies, a large real-estate firm, returned to the ER, where she waited another three hours.
“Finally, at 6 am I was put into triage and brought to a bed in an ER bay. By this time, I was feeling very weak. I was given an IV and fell asleep. I woke up an hour and a half later at about 7:30 am, and still no one had done an assessment of me. A nurse came in and drew some blood. I passed out, and I woke up and felt sick again. By this time, I’d been vomiting off and on for more than seven hours.”
By 10 am, more than eight hours after she arrived, Abramson—feeling better and able to keep apple juice down—was released from the ER. “As I walked through the waiting area, the young guy with the broken nose was still there. I waved to him and told him I was sorry, and he just shook his head.”
Other than a burst blood vessel in her eye from vomiting and weakness that lasted for a few days, Abramson recovered. She wanted to know her blood-test results to see if they identified the cause of her illness, but in the turmoil of the ER her blood samples apparently had not been sent to the lab for analysis.
“The doctors and nurses were all pleasant to me,” she said, “but they were understaffed and totally overwhelmed.”
Recounting Abramson’s experience is not meant to single out GW’s emergency department, which has a tradition of delivering good care. Rather, it illustrates what’s happening in hospital emergency departments more often. Every ER in the area is overcrowded and understaffed at times, and patients suffer the consequences. As one emergency physician says, “At one time or another, every emergency department runs into serious problems.”
Emergency medicine today is caught in a tug of war. It has made dramatic strides in quality of care in the past 25 years. Emergency rooms once were the province of moonlighting doctors who worked in the ER to make extra money, but emergency medicine has evolved into a recognized medical specialty that requires physicians to undergo extensive training and pass a rigorous board-certification examination.
But as Abramson’s story and others illustrate, hospital emergency departments face increasing problems. The result is that the medical safety net that treats people from all walks of life—the ill and injured, the uninsured who by law can’t be turned away, people with psychiatric, alcohol, or drug problems—seems in danger of collapse.
In December, the American College of Emergency Physicians (ACEP) released its annual report card on the state of emergency medicine. It gave the nation’s emergency-medicine system a C-minus overall and termed it a “ticking time bomb.”
The normally understated Institute of Medicine (IOM) subtitled its 2006 report on hospital-based emergency care, “At the Breaking Point.” Both reports underscore the increasingly distressed state of hospital emergency departments.
The numbers tell part of the story.
Between 1993 and 2003, the IOM report said that the population of the United States grew by 12 percent, hospital admissions increased by 13 percent, and emergency-department visits rose from 90 to 114 million—a 26 percent increase.
Over the same period, the United States experienced a net loss of 703 hospitals, 198,000 hospital beds, and 425 hospital emergency departments. Moreover, patients coming to ERs today are older and sicker and require more complex and time-consuming workups and treatments.
The nation’s hospital emergency system, ACEP said in its 2008 report, is “under more stress than ever before.”
The Washington area is following national trends, but the ER situation is better here than in many other places.
Hospital emergency-department visits are up across the region. In the District they rose from 366,673 in 2000 to 407,719 in 2007, an 11-percent increase—despite the loss of two emergency departments. DC General Hospital, which had 51,491 ED visits in 2000, closed in 2001. Hadley Memorial Hospital—now called the Specialty Hospital of Washington—which had more than 9,000 emergency visits in 2000, quit operating its emergency department.
Fourteen hospitals in the Maryland suburbs had 619,878 emergency visits in 2000 and 767,708 in 2007, an increase of about 25 percent.
Nine Northern Virginia hospitals reported 371,386 ED visits for 2000 and 442,291 in 2007—also up by almost 20 percent. Not included in those figures are four freestanding Inova-operated ER clinics in Reston, Loudoun County, Fairfax County, and the Springfield/Franconia HealthPlex. Visits to the HealthPlex nearly doubled, from 16,435 in 2001 to 31,739 in 2007.
Overall, the Washington area rated fairly well compared with the rest of the nation on ACEP’s emergency-care report card, which was based on 116 medical indicators in five categories—access to emergency care, quality and patient-safety environment, medical-liability environment, public-health and injury prevention, and disaster preparedness.
Both the District and Maryland earned all-around grades of B-minus, which placed them near the top nationally. No state received an A, Massachusetts was the only state to rate a B, and Rhode Island was the only state besides Maryland and DC to get a B-minus. Virginia earned a C.
The District was cited for having the highest percentage nationally of emergency physicians, surgeons, specialists, and registered nurses per 100,000 people. It was the only jurisdiction in the country to score an A for patient access to emergency care, a category in which Virginia got one of the lowest grades in the country, a D-minus.
The District got a C for quality and patient-safety environment based in part on the fact that DC had a low percentage of heart-attack patients (41 percent) who received angioplasty within 90 minutes of arrival at the ED. Maryland earned an A in this category, and Virginia received a C-plus. Virginia’s highest grade was a B-plus for disaster preparedness and a B for public health and injury prevention.
Dr. Thom Mayer generally agrees with the ACEP assessment for this area. Mayer is founder and CEO of BestPractices, an independent contractor that provides emergency physicians for Inova Fairfax, Inova Fairfax for Children, Potomac Hospital, Inova HealthPlex, and the Inova emergency-care centers in Reston and Fairfax. Private contractors help most area hospitals staff their emergency departments.

One problem more prevalent here than in some parts of the country is the chronic unavailability of on-call specialists such as neurosurgeons. This means that some patients who come into the ED with a serious medical emergency, be it a broken leg or stroke symptoms, may not be treated by a specialist.
A chief reason is what physicians see as a toxic medical-liability climate in the area. Says Dr. Robert Rothstein, director of emergency medical services at Suburban Hospital: “My on-call docs don’t want to take ER calls because they’re afraid to come in and see someone who is uninsured or drunk or who is not going to pay them and is likely to sue them. So what happens to the guy who breaks his ankle and comes to the ER and needs an orthopedic surgeon at 3 am? He’s not going to get one, at least not very easily.”
“You can’t pay enough money to on-call specialists to have them come into the ER and put themselves at that kind of liability risk,” says Dr. Mark Smith, chair of emergency medicine at Washington Hospital Center. “I’m not surprised we have a shortage of on-call physicians. I’m surprised we have any at all.”
The ACEP report card gave the District an F on its medical-liability environment, the lowest grade in the nation. Maryland got a D-minus, Virginia a C-minus. ACEP noted that the District has the second-highest incidence of malpractice awards—eight per 100,000 people—compared with a national average of 2.4 per 100,000. DC’s malpractice awards averaged $366,131 versus $285,218 nationally.
The average medical-malpractice award in Maryland is $319,977, nearly $35,000 more than the national average. The average medical-liability premium for specialists is $100,625, compared with the national average of $65,489. The report credited Virginia with making strides in medical-liability reform, such as requiring that expert witnesses be of the same specialty as the defendant, but said it needs more.
Virginia’s malpractice climate is likely part of the reason that emergency departments there generally have better access to on-call specialists. Says Dr. Martin Brown, chief of the emergency department at Inova Alexandria Hospital: “We have a large medical staff, and there’s a lot of loyalty.” The one exception, he says, is neurosurgeons. Brown says his ED transfers some neurological cases to Inova Fairfax Hospital, which has a neuroscience specialty center.
People without life-threatening emergencies often wait hours in emergency departments. That’s why some people do their best to avoid going to a hospital—and why others walk out before getting treatment. According to a Rand study of DC health and emergency care released in June 2008, the percentage of “leave without being seen” patients at seven DC hospitals ranged from 2.3 percent to 10 percent, compared with a national average of 1.3 percent.
Long waits are a touchy subject for hospitals—most won’t reveal how long patients wait for emergency treatment.
There are different ways to measure patient waiting times. One is to calculate the time it takes for a patient to see a physician; another is to measure the total time a patient spends in an ED. According to the ACEP report, the average waiting time nationally to see a doctor in emergency departments has more than doubled in the past decade to just less than one hour, and the average time spent by patients in an ED is four hours.
The Washingtonian asked every hospital in the area to disclose its ED waiting times. Most hospitals refused.
According to the Rand study, the median time patients wait in a DC emergency department before seeing a physician is 90 minutes, double the national average of 47 minutes. The median time from triage to discharge is 3.7 hours, 25 percent longer than the national average.
The consulting firm Press Ganey conducted a 2007 patient survey of ED experiences for 1,524,726 people in all 50 states but not the District. It found the average time patients spent in Maryland emergency departments was 275 minutes, or just more than 4½ hours. In Virginia, the average visit was four hours and 45 minutes. These were among the longest waiting times in the nation, with Maryland 42nd and Virginia 46th among the 50 states.
The ACEP report found that even patients experiencing pain or heart attack face delays. Researchers at Harvard Medical School reported that the median waiting time in hospital emergency departments for patients suffering “acute” heart attacks—when fast treatment is critical—increased from 8 to 20 minutes between 1997 and 2004. Waiting times likely are longer today.
“The emergency-care situation has gotten worse year after year,” says Washington Hospital Center’s Dr. Mark Smith, “and what really strikes me now is just how fragile the whole healthcare system has become. Everything has been squeezed out of it that can be squeezed, and we already are facing a space-and-capacity crisis. A bad flu season could be a catastrophe because we are operating on such a thin margin.”
Many already overburdened EDs have had to absorb some of the increased patient load caused by the closing of DC General Hospital, the District’s only public hospital, which served many indigent patients. Emergency departments at Providence and Howard University hospitals, Washington Hospital Center, and others have taken the brunt of the load.
DC General was where law-enforcement authorities took prisoners in need of care and where ambulance services took many drunk, unruly, or potentially violent patients. Now officials take these patients to other emergency departments.
“Hospitals have been running fuller since DC General closed,” says Dr. Smith, “and at times we’ve been in an overload situation. When that happens, you get degradation of service. This is not just happening here but in hospital EDs around the country.”
Patient Boarding—Lining the Halls
Emergency departments are major entry points for patient hospitalizations. Suburban Hospital reports that 74 percent of its inpatients come through the ED, whereas Inova Alexandria Hospital admits about a third of its patients through the ED. Logjams occur all too often because no inpatient beds are available, including intensive-care and critical-care beds.
This leads to patient “boarding”—of patients being kept in or around the ED until an inpatient bed becomes available. Boarding usually lasts an hour or two, but some patients linger in boarding limbo for a day or more. Even critically ill patients are boarded—they wait in hallway gurneys with IV lines running and ED nurses and doctors checking on them.
Boarding is a constant in emergency medicine, and it compromises patient care. Says one emergency physician: “If any hospital in the Washington area says they don’t board ED patients, they’re lying.”
The problem is exacerbated by the growing influx of psychiatric patients who either walk into an ED or are brought by police or family members because there’s nowhere else to go. They come with such problems as drug and alcohol abuse, depression, homelessness, hallucinations, and suicide attempts.
Of the 328 emergency-department directors who responded to a 2008 ACEP survey, 80 percent said they boarded psychiatric patients. The Washington area is no exception.
“Psychiatric patients are a major problem in the emergency department because we have fewer and fewer psychiatric beds available,” says Suburban Hospital’s Dr. Robert Rothstein. “Some psych patients spend two, three, even seven days in an ER waiting for a bed that’s appropriate for them. These are patients who don’t always need to be in an ER, but community resources for them are just not available. Nobody follows them up, and they are often cast adrift with no place to go. There is involuntary commitment, but the way the laws are written, that is very tough to do.”
Dr. Bob Cates, chair of emergency medicine at Inova Fairfax Hospital, says his department sees about 250 psychiatric patients a month, sometimes for minor problems such as insomnia but at times for significant psychiatric problems that emergency physicians attempt to stabilize with medication. Cates says many local hospitals have closed their psych units, leaving the few that will accommodate psychiatric patients to handle a greater load.
Says Cates: “I know of at least three area hospitals that have shut their doors to psychiatric patients.”
In a survey of nearly 90 hospitals around the country conducted on a typical Monday evening, 73 percent reported boarding two or more patients at that time. On random afternoon visits to several Washington-area EDs, all had boarders. The average ED boarding time in DC hospitals ranges from two to eight hours, according to the Rand report, a number some ED doctors think is too low.
Patient boarding stretches emergency personnel thin and was likely part of the reason for the delays experienced by Marnie Abramson, the patient who spent more than eight hours in GW hospital’s ER.
“Boarding not only compromises the patient’s hospital experience,” the IOM report said, “but also . . . enhances the potential for errors, delays in treatment, and diminished quality of care.” One study on boarding found a higher death rate for patients boarded more than six hours in the ED, and another showed that elderly patients who were boarded longer than six hours were more than four times as likely to end up in nursing homes than return to their own homes after leaving the hospital.
Says Dr. Robert Rothstein: “We’re keeping people in the emergency departments for hours if not days. We’re doing critical care in the emergency department, which is not what we’re meant to do.”
“When we admit ED patients and board them in the ED area,” says Dr. Mark Smith, “we’re taking care of them at the same time more patients are coming through the door. Sometimes you are boarding 25 or even 35 of these patients up to 36 or 48 hours and your staff is stretched thin caring both for them and the new patients.”
Dr. Cates of Inova Fairfax Hospital, which saw more than 65,000 ED patients in 2008, says, “If we have an ill patient we’re boarding, guess what ED nurses are going to be doing? They’re going to be taking care of the boarding patient and not the patients coming through the door. So a major initiative of our hospitals is how to better handle boarders.”
Dr. Rothstein recalls a grandfather lying in a gurney outside the ER for 14 hours: “I told the family there were no beds available at our hospital or any of the other nearby hospitals, so we could not transfer him anywhere else. They were incredulous, but this is the kind of thing that routinely goes on in emergency departments today.”
Boarding isn’t always the result of too few hospital beds but rather of too few staffed beds.
Says one area physician: “Think of it as a barbershop. If you have three chairs and see 90 customers a day, each barber cuts 30 heads of hair. If you go to six chairs, customers won’t wait as long to get a haircut, but now you’re paying six barbers instead of three. That’s how hospitals think. It’s not a customer-service model they follow; it’s a utilization model.”
Writing in Slate.com in July 2008, Drs. Zachary F. Meisel and Jesse M. Pines, both emergency physicians and senior fellows at the Leonard Davis Institute of Health Economics, pointed out one way that boarding helps tamp down hospital costs.
“Hospitals generally maintain strict patient-to-nurse ratios for inpatients,” they wrote. “But many hospitals don’t apply the same rules to the ER because they can’t control the number of patients who come in that way. Sometimes the patient to nurse ratio in the ER can be as high as 8-to-1. That’s unacceptable in inpatient units, but just stack ’em in the ER hallways and suddenly it’s OK.”
Nurse-to-patient ratios are important. A study published in 2002 in the Journal of the American Medical Association found increased risk of patient mortality when one nurse cares for more than four hospital patients. The chances of nurse burnout also increase significantly when nurse-to-patient ratios are higher than one to four.
ED physicians agree that boarding is harmful for patient care. But for now it’s a fact of life.
Diversion—When the ER Is Full
On a February afternoon in 2008, Brandy Nannini received a call. Her daughter’s nanny told her that two-year-old Bella was suffering a seizure.
Nannini—vice president for government relations at the Century Council, an Arlington-based nonprofit that targets drunk driving and underage drinking—told the nanny to call 911 for the Arlington emergency medical service while she phoned Bella’s neurologist. Bella had a genetic disorder that made her susceptible to seizures. She had suffered them before, but always when Nannini was at home.
“This was a very scary situation,” Nannini says. “Bella loses her muscle tone and turns blue when she seizes because she doesn’t get enough oxygen.”
Nannini reached the neurologist, who asked her to tell the ambulance to take Bella to Georgetown University Hospital’s emergency room, where he would meet them. Nannini relayed this to the EMS squad, who initially agreed but then got back to her.
“The EMS people told me they could not take Bella to Georgetown because the emergency room there had gone on diversion,” Nannini says. “I couldn’t believe it. I’d never heard of hospital diversion before.”
Knowing that every passing minute meant Bella could suffer brain damage, Nannini called Georgetown’s ED. She said Bella’s neurologist was to meet her there and pleaded for the hospital to take her. Because of a flu virus going around, Georgetown, like other area EDs, was overflowing with patients; Nannini was told the hospital had no space to treat Bella.
By this time, Nannini’s husband, Michael, had arrived home from his job as an associate at Booz Allen Hamilton. He got into the ambulance with his daughter, and it took them to Inova Alexandria Hospital. Bella had nearly turned blue from oxygen deprivation; the EMS crew administered oxygen on the way to the hospital, and her pink color began to return.
Brandy Nannini met her husband and Bella at the hospital and was stunned by how crowded the ED was. “There were people lying on gurneys lining the hallways,” she says. “The place was absolutely jammed. I thought, with people’s lives at stake, this is crazy.”
Realizing Bella needed immediate medical attention, nurses quickly took her to an emergency bay, where treatment controlled her seizures.
Because they wanted the neurologist to see Bella, the Nanninis arranged for her to be transferred to Georgetown a few hours later. They arrived late at night and found the ED as crowded as the one at Alexandria.
“The Georgetown emergency room was filled with people, and there were gurneys in the halls there, too,” Nannini says. “Some of the people looked like they had the flu, others were there with broken bones, and some were drunk enough that you could smell the alcohol.”
Bella needed to be admitted as an inpatient; by midnight she finally was settled in the last available bed in the pediatric-neurology unit.
The Nanninis’ experience is part of a growing pattern. When a hospital can’t accept emergency patients, it transmits this information to EMS ambulance crews, who then “divert” patients from that hospital to another. ED directors say they resist going on diversion but at times are forced to because their departments are overwhelmed.
“We feel an obligation to the community to remain open, so diversion is something we don’t want to do unless it is absolutely necessary,” says Suburban’s Rothstein. “We don’t do it very much, but there are times we have to.”
An obvious concern about diversion is that it can cause potentially catastrophic delays for patients who have to be transported to a hospital farther away. Fortunately for Bella, there is no evidence of permanent damage caused by the diversion from Georgetown.
Diversion is directly linked to patient boarding and is a problem in all area jurisdictions. DC Fire and Emergency Medical Services (FEMS) chief Dennis Rubin says diversion causes ambulances to be rerouted and also can tie them up at hospitals for long periods, causing a shortage of vehicles for other emergency runs.
“There’s been a significant increase in hospital diversion in the past five years,” says assistant EMS chief Mike McAdams of the Montgomery County Fire and Rescue Service, “and it really stresses the EMS system. I normally have a cycle time of 45 minutes from patient pickup to leaving the ER, but when we’re on diversion, all of a sudden the cycle time lengthens, and this makes for less availability of EMS vehicles.”
Ned Sherburne, chief of the Bethesda–Chevy Chase Rescue Squad, says diversion is not the only issue: “We have had a much more significant problem when hospitals don’t go on diversion and in-bound ambulances are held hostage by ED nurses and physicians who refuse to move patients to hospital stretchers and use ambulances to board their patients. I have had units held as long as several hours.”
“Diversion pushes the burden on other hospitals and has a domino effect,” Montgomery County’s McAdams says. “Ambulances get stacked up because they can’t unload their patient at the ER. Once when Shady Grove Adventist went on diversion, we had eight ambulances backed up at Montgomery General. Sometimes ambulances have to wait 45 minutes or longer to unload a patient, and that can throw off the system to the point that we have to pull ambulances from one area to cover for another.”
Baltimore recently ran out of available ambulances because they were tied up waiting to unload patients at overcrowded EDs, says Dr. Robert Bass, executive director of the Maryland Institute for Emergency Medical Systems Services (MIEMSS), which oversees the state’s emergency system.
EMS providers in DC and its suburbs transport emergency patients across jurisdictional lines when hospital EDs in their area are at capacity. District EMS sometimes transports patients to Maryland hospitals, such as Prince George’s Medical Center, and they also occasionally transport diverted patients to Alexandria, Mount Vernon, and Arlington hospitals in Virginia.
“It can go both ways,” says Melinda Duncan, executive director of the Northern Virginia EMS Council. “Arlington and Alexandria EMS at times transport patients to George Washington.”
Even when an ED is on diversion, it can accept patients with life-threatening conditions and provide initial stabilization before the patient is transported to another facility.
ED diversion times for Maryland and DC hospitals increased dramatically from 2002 through 2007. According to figures supplied by the District’s Fire and Emergency Medical Services, DC hospitals went on diversion a total of 7,668 hours in 2003; in 2007, the total was 13,991, an increase of 83 percent. In 2008, the District FEMS reports, diversion hours dropped to 8,843 as both EMS and District hospitals made a concerted effort to cut down on diversion.
In Maryland, MIEMSS counts diversion time differently than DC FEMS, totaling hours for each diversion category, or code. EDs go on red alert when they have no available cardiac-care beds and on yellow alert when they’re too full to accept general-care patients; a “mini-disaster” means a hospital is experiencing a power outage or other problem that prevents it from accepting emergency patients. This method of compiling hours by code hours rather than clock hours yields a much higher total than DC’s method.
According to MIEMSS, hospitals in Maryland’s Region V—which includes Montgomery, Prince George’s, Charles, Calvert, and St. Mary’s counties—went from a total of 18,348 ED diversion hours in 2002 to 30,047, or 64 percent more, in 2007. Figures available for 2008 indicate a decline to around 18,000, suggesting improvement in Maryland, too.
Diversion hours for Northern Virginia hospital EDs are not disclosed by public authorities. Despite several requests, the six Inova hospitals refused to disclose the diversion hours of their EDs, and hospitals that did so generally reported low numbers. But the low numbers may be suspect, say Northern Virginia EMS officers—likely a result of how the hospitals define “diversion.” Says one emergency physician: “I guarantee you that all hospitals in Northern Virginia are diverting ED patients.”
Melinda Duncan says EMS providers in Northern Virginia report that diversion is increasing there, too. “If our EMS providers think a patient can safely go to another hospital ten minutes more down the road, they’ll take him there,” she says, “but sometimes patients go from stable to unstable very quickly. When this happens, EMS providers are concerned not only for the patient but from a liability standpoint as well.”
Easing Boarding and Diversion
There’s no way to reduce the number of people going to emergency departments today or suddenly to open up hundreds of new hospital beds, though some area hospitals do plan to increase their ED capacity over the next five years.
But studies suggest ways to ease waiting times, patient boarding, and diversion without expanding ED capacity.
“It sounds paradoxical, but studies in the IOM report found little correlation between the number of people coming into the ER and the need for hospitals to go on diversion,” says MIEMSS’s Dr. Bass. “The most likely predictor for a hospital going on diversion was the number of elective procedures it performed that day. This is because ED patients can’t be admitted when elective surgical patients are occupying ICU and floor beds, so the ED boards these patients and as a consequence becomes too crowded and understaffed.”
Studies have linked ED boarding and diversion to the fact that many inpatient beds are taken by elective-surgery patients. Because elective surgeries are usually performed early in the week, some experts recommend that hospitals have their surgeons schedule elective surgeries more evenly throughout the week to help improve patient flow and to free more inpatient beds.
The discharging of hospital patients is also an issue. Duncan says doctors need to make hospital rounds in the morning so they can discharge patients earlier and open up inpatient beds.
Says Dr. Eric Glasser, an emergency physician at Georgetown hospital: “Another factor is how quickly the housekeeping staff can turn an inpatient bed over so it will be ready for a new patient. If we could get ER patients upstairs faster, we could handle what’s coming into the ER better and reduce the need to board patients or go on diversion. To do this, we need commitment from top to bottom because diversion is a warning sign that tells us there is a hospitalwide problem, not just an ER problem.”
Cindy Notobartolo, corporate director of ED safety-and-security services at Suburban Hospital, says turning over inpatient beds faster and earlier in the day is not as easy as it might appear. In the past, she says, patients frequently were discharged at noon, but now family members are often working and unable to take patients home until late in the day. Some patients also wait long periods for private ambulances to transfer them to extended-care facilities. Delays also can occur because a bed becomes available in a semiprivate room with a male patient but the ED patient in need of a bed is female.
It might seem that hospitals could at least demand that surgeons change their operating schedules to maximize the number of open beds in the afternoon and evening, peak ED times. But hospitals rely on surgeons to bring in patients, so they generally try to accommodate them. As a 2003 General Accounting Office report pointed out, “hospitals often balance admissions from emergency departments with scheduled admissions for surgical procedures, which are generally considered more profitable.” In addition, more ED patients than elective surgical patients are uninsured or underinsured.
Information technology may help EDs work more efficiently. Most EDs in the area now have electronic patient records. This means that an ED physician can gain quick access to a patient’s medical records, but if the patient was previously seen at another hospital, the physician must submit a special form to gain access to those records, a time-consuming process.
BestPractices’ Dr. Thom Mayer says hospital EDs also need to institute common-sense ways to deliver care more promptly. “When you go to the ER,” he says, “registration asks you to come up, then you go back to the waiting room. You are usually seen by triage and asked questions, and then a nurse calls you back into the ER and asks you the same questions you were asked at registration and triage. Then the doctor comes in and asks the same questions again. It makes no sense. Why don’t we take patients directly into the ER and register them there? We do this all the time with heart attacks and trauma, and we should apply it to the more routine complaints to speed the process.”
Mayer also says people who come into the ED don’t always need a bed, just a place to sit, and that patients who remain upright are likely to be treated faster and to leave faster.
“We have to keeping asking ourselves: Why do we keep doing it this way, and is there another way to do it?” he says. “We need to be open to new ways of doing things both clinically and from a customer-service standpoint. I think this will happen, and I think you’ll see great EDs will help show the way because every major trend in healthcare is first seen in the ED.”
The emergency-medicine crisis needs innovation if we are to shorten patient waiting times, provide better care, and free EMS providers to respond to emergency calls faster. When this happens, the story of a sixtyish woman we’ll call Diane could become much more common than Marnie Abramson’s.
“I began experiencing mild chest pain and tingling down my left arm in the morning, and it continued into early afternoon,” Diane recalls. “I asked my husband to take me to an emergency room.” When she arrived at 3 pm, there were no more than five or six people in the waiting area, surprisingly few for that time of day—late afternoons and evenings are usually the busiest times in emergency departments. Diane described her symptoms at the registration desk. Without delay, a nurse escorted her to an ER bed and attached leads from an electrocardiogram (ECG) to her arms, legs, and chest.
An ER physician saw her within a short time and called in a cardiologist, who read the ECG. The ECG didn’t register signs of a heart attack, but given Diane’s age and symptoms, the cardiologist, to be cautious, asked her to remain under observation in the ER. Blood was drawn, and tests showed a slight increase in enzyme levels that could be associated with heart attack, but they were within the high-normal range.
Diane’s symptoms eased somewhat, but the cardiologist wanted to admit her to the hospital for overnight observation. People complaining of heart-attack symptoms have been released from EDs when no evidence of a heart attack was detected, only to suffer heart attacks a short while later.
Orderlies wheeled Diane upstairs to an inpatient bed, and she wore a heart monitor all night. The cardiologist gave her a treadmill stress ECG test the next morning. Findings from both studies were normal, and Diane was released that day. The tingling in her arm returned off and on; a neurologist later determined that it was likely caused by carpal-tunnel syndrome. Diane now wears a wrist brace at night, and the tingling has abated.
“From the moment I first spoke to the ER receptionist,” Diane says, “I felt I was very carefully monitored and whatever medical care I might need would be given immediately. I felt very safe and in very competent and caring medical hands.”
The experiences of Marnie Abramson and Diane could not be more different—but both occurred in the George Washington University Hospital emergency department within a few months of each other.
In emergency care, as in much of life, timing can be everything.
This article first appeared in the April 2009 issue of The Washingtonian. For more articles from that issue, click here.