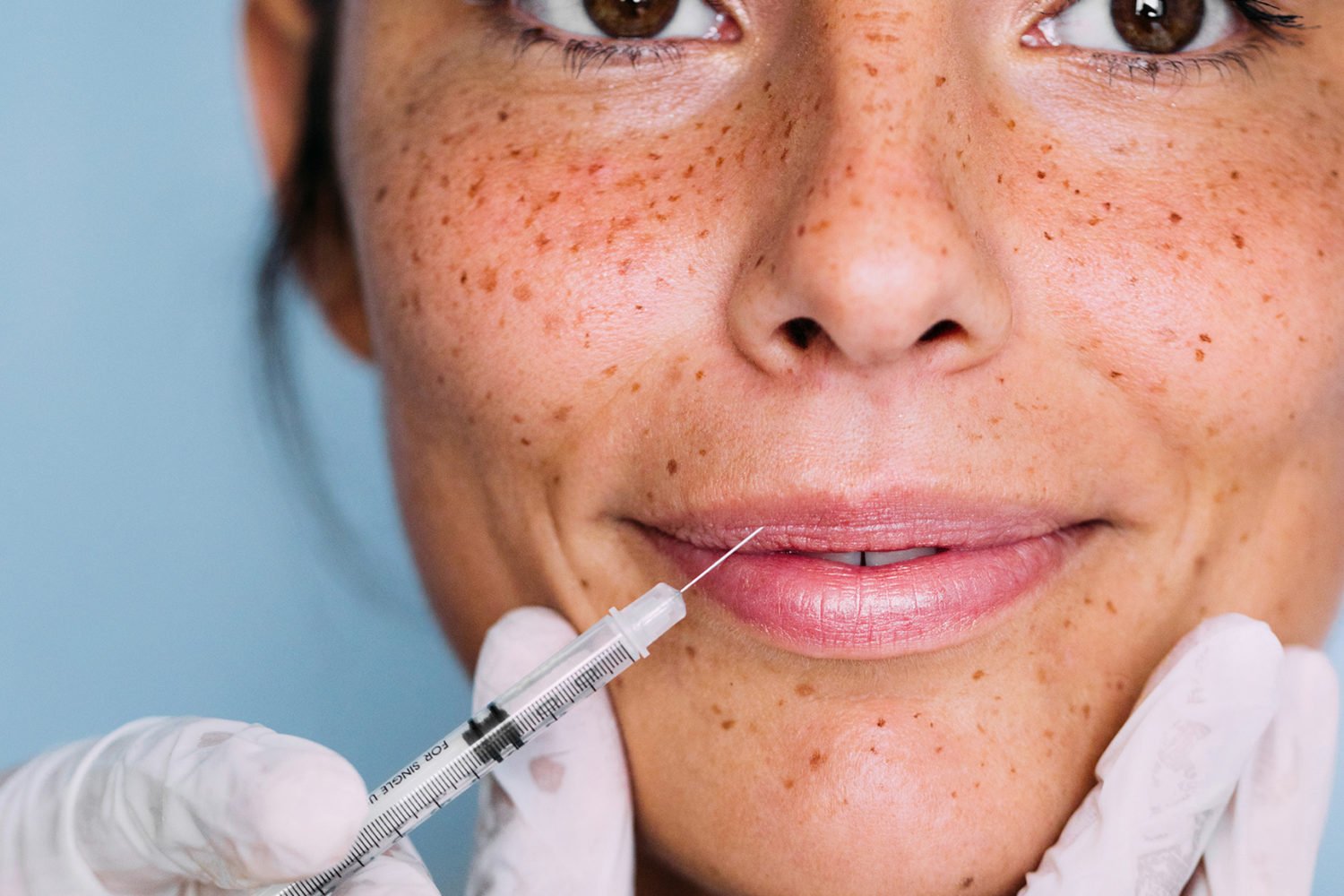
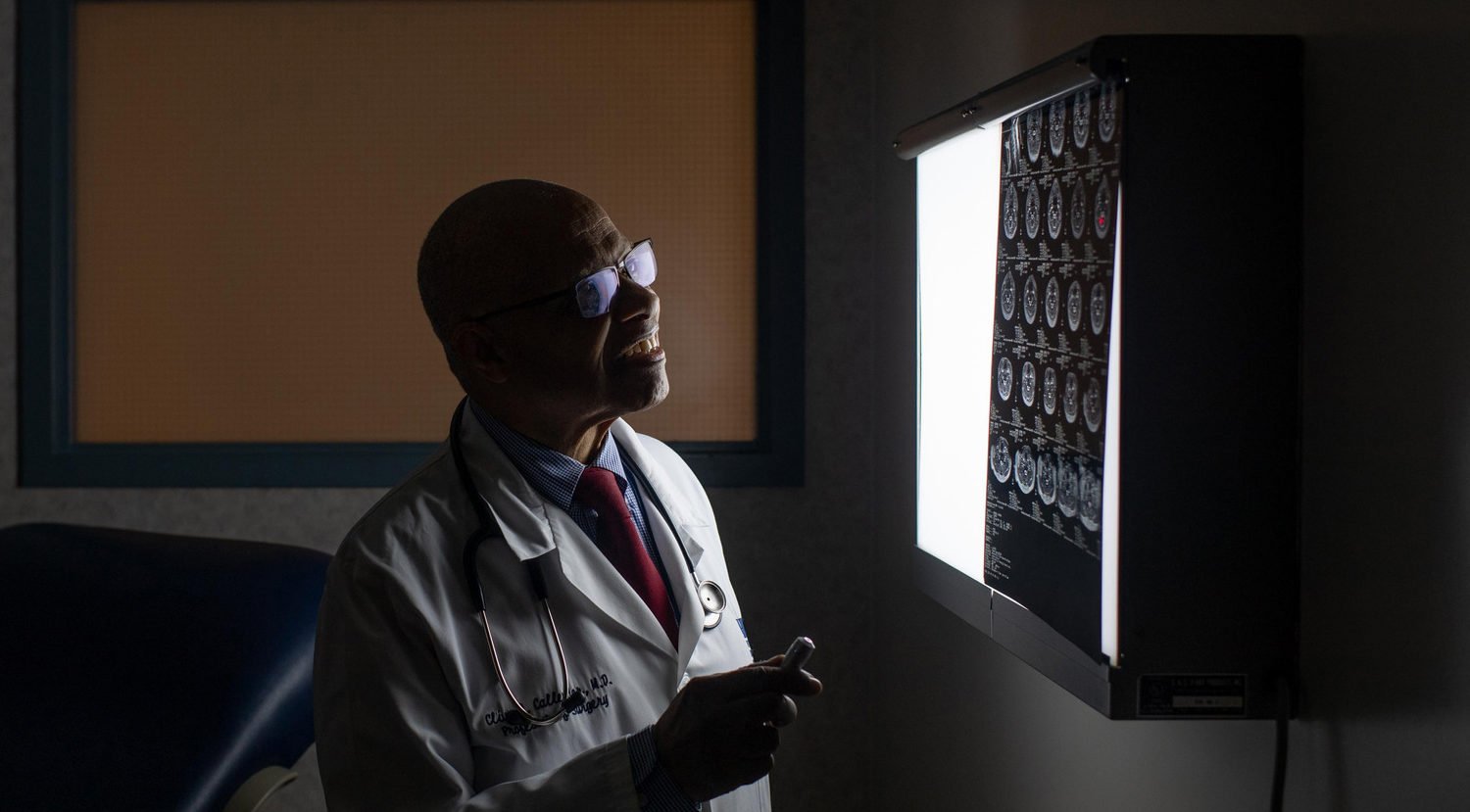
Doctors see their patients at some of the most vulnerable and painful moments of their lives. And while their bedside manner might remain stoic, a recent study suggests those moments can alter the decisions they make as medical professionals.
Comments from a group of oncologists who were interviewed for the study showed that after a patient’s death, doctors can experience such grief that their subsequent treatment decisions for other patients are affected.
The study, which researchers said was the first of its kind, involved 20 Canadian oncologists interviewed between November 2010 and July 2011. Trainees and junior and senior oncologists were included.
Researchers found that due to oncologists’ typically close relationships with cancer patients, their grief spills over into other areas of their lives, on both a career level and a personal one. “Oncologists’ grief had unique elements related to their sense of responsibility for their patients’ lives,” researchers noted.
The doctors interviewed for the study said they felt feelings of failure, powerlessness, and guilt when a patient died in their care. One said, “Let’s face it, people who go into medicine have full-blown fantasies [ . . . ]. You think you’re going to go in there to cure people [ . . . ] and it doesn’t happen. Sometimes I make an impact on what happens, but sometimes I just get steamrolled.”
Another said, “Sometimes I cry. I cry on the way home in the car.”
One local oncologist not involved with the study, Dr. Robert Hong of Virginia Hospital Center, says the field of oncology experiences a high burnout rate because “you can’t just shake off what you’ve experienced and all the hard work you put in during the day. It doesn’t turn off like a light switch. For me, I think about my patients constantly, whether I’m at home, at dinner, or at church.”
Hong says the most concerning results of the study were that oncologists admitted a patient’s death can lead to a negative impact on treatment decisions. One oncologist was quoted as saying, “Maybe I got that case after someone had just died and I was in a more aggressive mode. Or maybe I undertreated someone because I just saw a patient with terrible toxicity [ . . . ]. It’s not a science; it’s very much influenced by a lot of things that are very difficult to quantify.”
In an editorial to the New York Times, one of the study’s researchers, health psychologist Leeat Granek, wrote that the doctors’ comments shed light on an ignored aspect of medical training: “Oncologists are not trained to deal with their own grief, and they need to be. In addition to providing such training, we need to normalize death and grief as a natural part of life, especially in medical settings.”
However, Hong says most medical schools, “at least in the US, have helped prepare us for dealing with these types of situations. [ . . . ] In fact, dealing with the death of a patient helps motivate me to get better and work harder toward a better outcome for similar patients in the future.”
And with a study that involved such a small population, Hong says the results may be a bit too generalizing. “Every individual doctor handles grief so differently,” he says. “It’s important to bring it to the forefront, and I think it’s an important study, but there’s a high variability from doctor to doctor.”
The full study is available on the Journal of the American Medical Association’s website.